Scaly skin can occur on any part of the body. It is usually a symptom of dry skin and is common on the arms, thighs and lower legs. Inflammation, itching and irritation increase the turnover rate of skin cells which leads to the formation of scales.
What Causes Flaky Skin?
It can be caused by a myriad of reasons. Below are some of them:
1. Natural Causes
It can be caused by the environment of various natural processes. These include dry climates, normal aging and indoor heating.
2. Habitual Causes
You can also get dry flaky skin as a result of your hygiene and lifestyle. This includes not taking a shower as often as you should, bathing with hot water, harmful ingredients in soap and personal care products, insufficient intake of water, wearing fabrics that irritate your skin and excessive use of soap when taking a shower.
3. Psoriasis
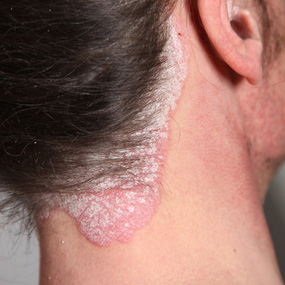 Psoriasis is a condition whereby the cells of your skin mature about 5 times faster than normal. Instead of the skin sloughing off naturally, it piles up on the surface of the skin forming a scaly structure. The cause of psoriasis is still a mystery to date. The symptoms of psoriasis include:
Psoriasis is a condition whereby the cells of your skin mature about 5 times faster than normal. Instead of the skin sloughing off naturally, it piles up on the surface of the skin forming a scaly structure. The cause of psoriasis is still a mystery to date. The symptoms of psoriasis include:
- Itchy scaly skin on the knees, scalp, elbows and upper body
- If you have it on your nails, the nails can become discolored, pitted and thick. They may also separate from the nail bed.
- If you have pustular psoriasis, you’ll have cracked, red, flaky skin with pustules on the palms of the hands or feet.
4. Eczema
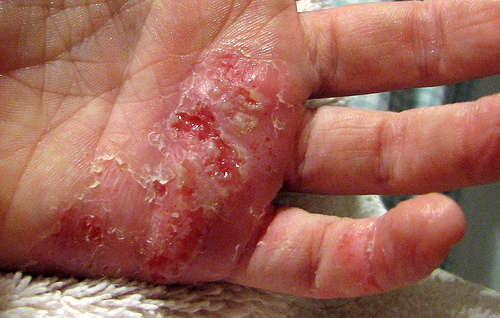 Eczema is a medical condition that causes the skin to become irritated or inflamed. There are several types of eczema with the most common one being atopic eczema. Eczema affects about 20% of infants and 3% of adults in the U.S.A. Eczema often starts off with itching followed by a rash. There are 3 types of eczema namely – atopic, discoid and varicose.
Eczema is a medical condition that causes the skin to become irritated or inflamed. There are several types of eczema with the most common one being atopic eczema. Eczema affects about 20% of infants and 3% of adults in the U.S.A. Eczema often starts off with itching followed by a rash. There are 3 types of eczema namely – atopic, discoid and varicose.
The affected skin usually appears very dry, or scaly and thickened. If you have fair skin, these areas may initially appear reddish and then turn brown. For people with darker skin, it can make the affected area either darker or lighter.
5. Is It Ichthyosis?
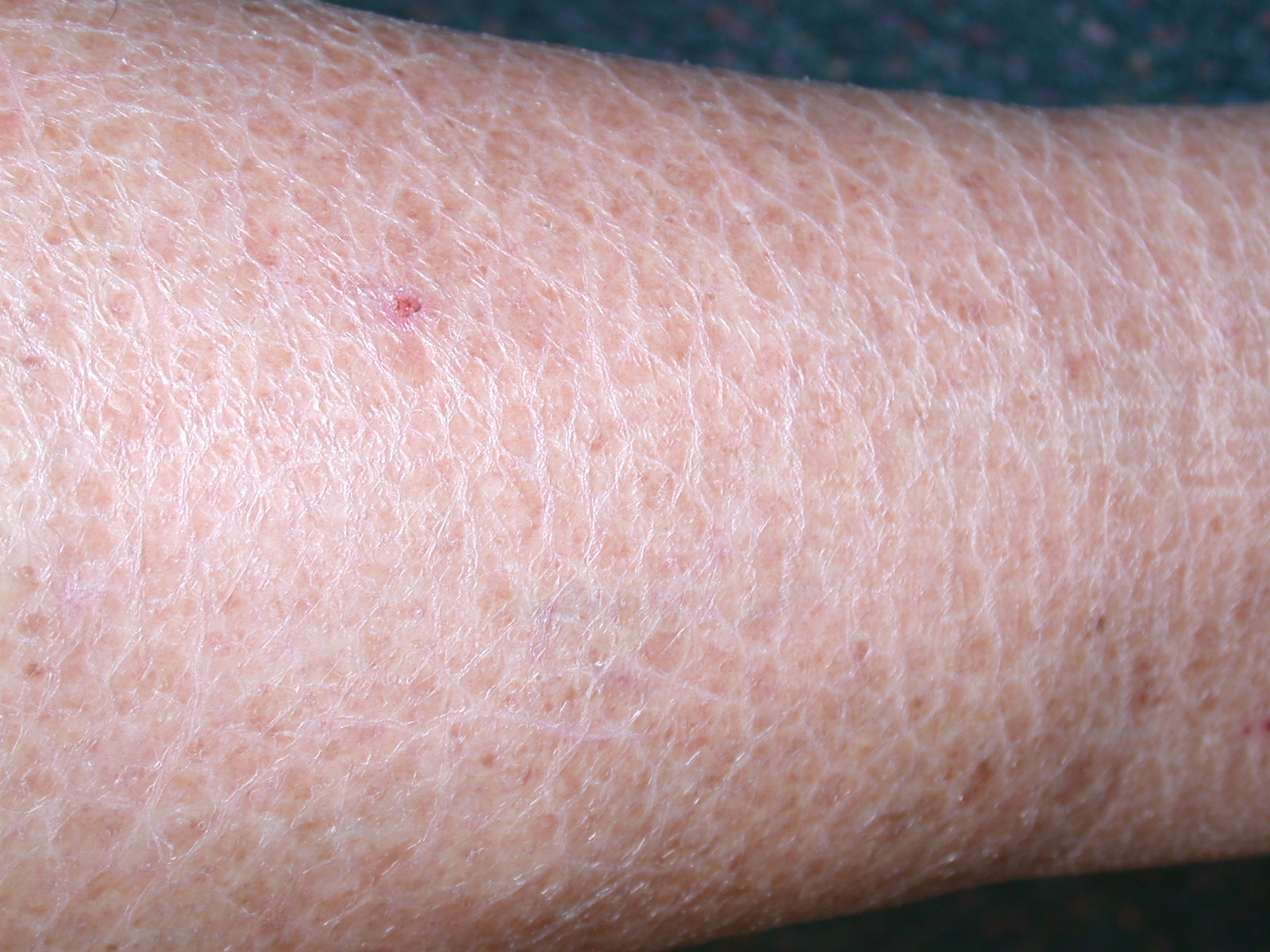 Ichthyosis vulgaris is a skin condition that is passed down in family. It is characterized by dry, scaly skin and is one of the most common skin disorders. It often begins in early childhood and is inherited in an autosomal dominant pattern. This means that you can get it by inheriting the abnormal gene from one parent. The symptoms include dry, flaky skin accompanied by mild itching. You could also experience mild skin thickening.
Ichthyosis vulgaris is a skin condition that is passed down in family. It is characterized by dry, scaly skin and is one of the most common skin disorders. It often begins in early childhood and is inherited in an autosomal dominant pattern. This means that you can get it by inheriting the abnormal gene from one parent. The symptoms include dry, flaky skin accompanied by mild itching. You could also experience mild skin thickening.
6. Other Causes
Sunburns can cause flaky skin, even the least severe cases. Some medications such as those for treating acne can cause the skin to peel. Chemotherapy medications can also cause peeling of the skin. Conditions that result in the formation of a blister can also cause flaky skin. There are cases where a skin infection can produce a rash or patches of flaky skin, e.g. impetigo, ringworms and allergic reactions.
How to Deal with Scaly Skin
|
Remedies |
What to Do |
|
Take anti-itch or allergy medication |
This includes non-prescription antihistamines such as cetirizine. If itching is severe, you can take diphenhydramine. |
|
Use anti-itch cream on the affected area |
You can use a non-prescription cream containing about 1% hydrocortisone to help relieve the itching. |
|
Moisturize your skin |
Immediately after taking a shower, apply moisturizer all over your body while you’re still damp. You can use oil or lubricating cream if your skin is too dry. |
|
Avoid scratching the affected area |
Try your best to avoid scratching despite the urge. You can cover the area with a bandage and wear gloves while you sleep at night |
|
Treat anxiety and stress |
Emotional disorders such as stress can aggravate atopic dermatitis. Improving your emotional health is, therefore, vital. |
|
Expose your skin to the right amount of sunlight |
You can improve skin lesions with a controlled amount of sunlight. Overexposure to sunlight can worsen the condition of your skin. Seek the advice of your doctor before starting a sunbathing program. Make sure to use sunscreen every time. |
|
Avoid alcohol |
If you are under treatment for psoriasis, you should steer clear of alcohol as it can interfere with the effectiveness of the treatment. |
|
Bathing
|
It is important to bathe every day. However, you should note that bathing strips your skin of its natural grease. If your skin is too dry, you should consider bathing only twice a week. You should also avoid drying or perfumed soap. |
|
Use humidifier |
Dry or hot air can worsen itching and flaking. A home humidifier adds moisture to the air inside your home. |
When to See a Doctor
Should the condition of your skin fail to improve or even get worse, you should see a doctor. Watch out for accompanying symptoms such as redness, fever or enlargement of lymph nodes. They could be a sign of a life-threatening condition.
